Unprecedented healthcare expertise
We help lawyers with their most challenging cases

Thousands of Cases
99% Success Rate
Our Mission
We are Healthcare
Unbiased Expertise
Our Commitment
Our Resources
We’ve helped thousands of firms win cases and increase their awards
0+
Thousands of cases
0+
Medical Experts
0%
plus expert engagement success rate
0+
Commercial Litigation
0k
Staff physicians at your service
0%
5-Star Trustpilot reviews
What success with Connect MLX looks like

The inside scoop on hospital triage
Connect Experts explores the system used by nurses to assess and priorize ER patients
It’s another packed evening in the hospital emergency room. You’re here with a painful cut on your hand, caused when you grabbed at a razor-sharp piece of falling metal tubing. You can’t help but notice that the busy waiting area is overflowing with patients and worried family members in equally dire straits.
Next to you, a mom sits anxiously with her toddler, whose tears, flushed face and bleary eyes suggest she has a fever. Across the aisle, an elderly man is coughing loudly into a tissue (causing you to secretly hope his illness isn’t contagious).
You’re called by the triage nurse, who tells you your swollen purple index finger should have been stitched days ago. She sends you back to the waiting room, smiling patiently as you ask how long until you see a doctor. “We’ll get you in as soon as possible, we have a lot of sick patients here tonight.”
Now, picture that you are the triage nurse for a moment. How do you determine who goes in next? Over the past 20 minutes alone, the following patients have arrived in the emergency along with the sobbing toddler with a temperature of 39.5C, a heart rate of 120/minute, sore throat and earache:

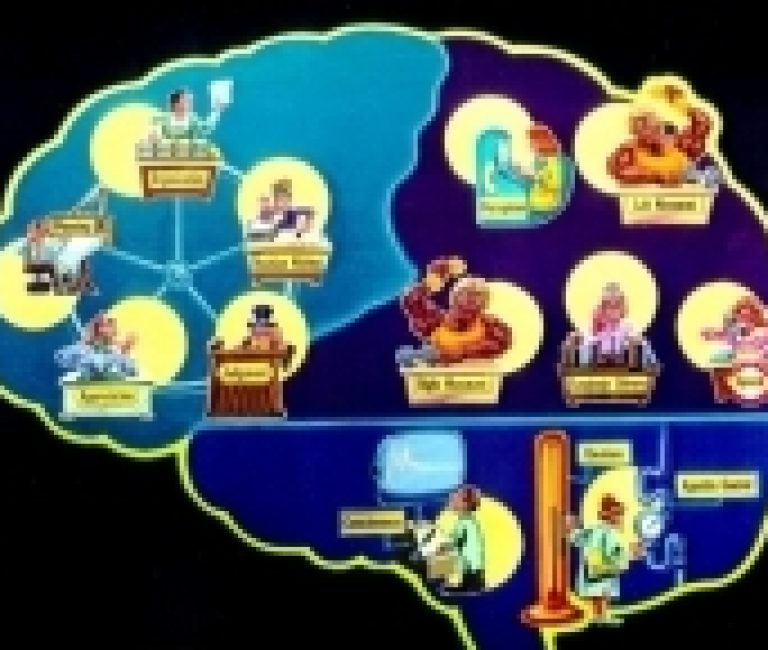
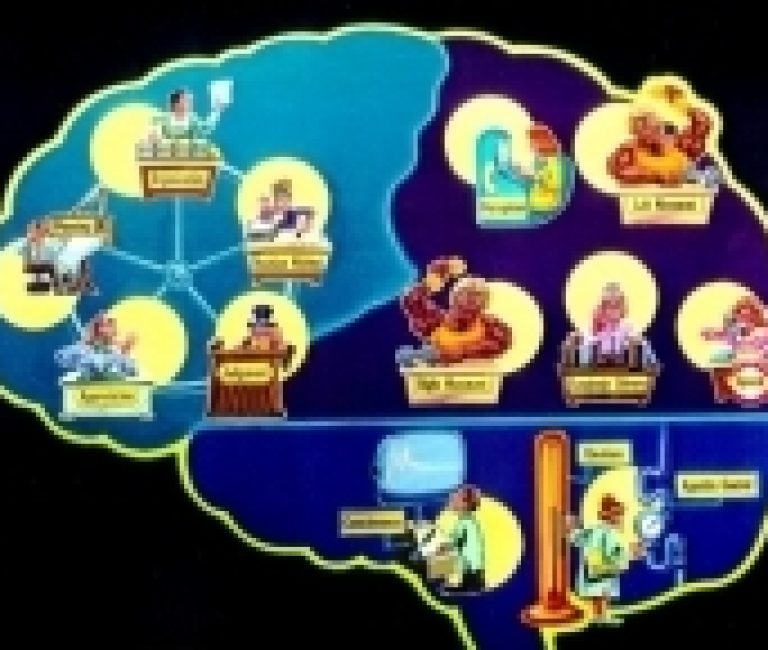
This white paper is the second of three parts on the complex functions of brain, what happens when an injury is acquired and how to care for and manage a life-changing brain injury.
BY LINDA SIMMONS, RN BScN
Consultant and Cost of Future Care Expert, Connect Medical Legal Experts
TBI refers to any injury to the scalp, skull (cranium or facial bones) or the brain. Injury to the brain can be focal or diffuse. Focal injuries result in contusions, lacerations, or hemorrhages. The hemorrhages that can occur are epidural hematoma, subdural hematoma, intracerebral hematoma, and subarachnoid hemorrhage. The diffuse injury can cause a mild to severe concussion or diffuse axonal injury.
This white paper is the first of three parts on the complex functions of brain, what happens when an injury is acquired and how to care for and manage a life-changing brain injury.
BY LINDA SIMMONS, RN BScN
Senior Nurse Life Care Planner, Connect Medical Legal Experts
This document will increase the health care professionals understanding of Acquired Brain Injury (ABI). ABI is defined as damage to the brain that is acquired after birth. It can affect cognitive, physical, emotional, social, or independent functioning. ABI is an umbrella term used to describe all brain injuries. ABI can result from traumatic brain injury (i.e. accidents, falls, assaults, etc.) and non-traumatic brain injury (i.e. stroke, brain tumours, infection, poisoning, hypoxia, ischemia or substance abuse).
The motor vehicle related accident clients that we at Connect Experts see with ABI have often resulted from a Traumatic Brain Injury and thus ABI’s that have resulted from a TBI will be the focus of this document.
What Our Clients Have To Say
As you recall, I came to you a few weeks ago, desperate for an expert to respond to a late-served defence opinion. The assignment was..
Aleks Mladenovic
Connect Experts Class Action Support Service has the qualities that matter to the legal community, Their team of experts are capable, timely and effective in..
Ray Wagner
I’m hooked. I won’t start an action without first obtaining the case merit review from Connect Experts.
Kevin Toner
Chris and her colleagues have helped our office many times in locating leading experts in specialized and sub-specialized areas of medicine, in sourcing medical information..
Joseph Miller K.C.
Connect with an expert witness